 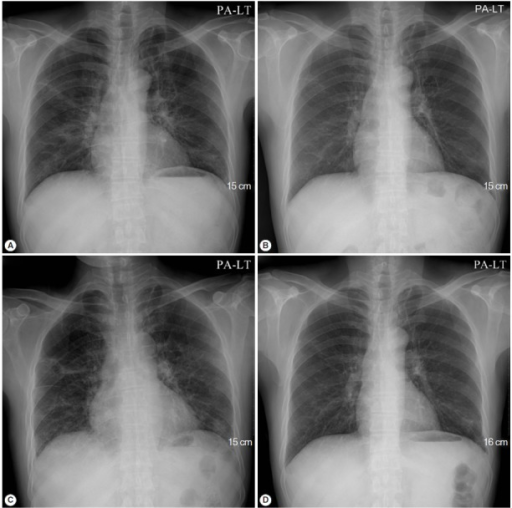
The fungus appears to be present in healthy individuals in the general population. jirovecii in lung fluids does not mean that a person has PCP or infection by HIV. Notably, simple molecular detection of P. Pneumocystis infection can also be diagnosed by immunofluorescent or histochemical staining of the specimen, and more recently by molecular analysis of polymerase chain reaction products comparing DNA samples. Both the thickened septa and the fluffy exudate contribute to dysfunctional diffusion capacity that is characteristic of this pneumonia. A lung biopsy would show thickened alveolar septa with fluffy eosinophilic exudate in the alveoli. The cysts resemble crushed ping-pong balls and are present in aggregates of two to eight (and not to be confused with Histoplasma or Cryptococcus, which typically do not form aggregates of spores or cells). Staining with toluidine blue, silver stain, periodic acid-Schiff stain, or an immunofluorescence assay shows the characteristic cysts. The diagnosis can be definitively confirmed by histological identification of the causative organism in sputum or bronchoalveolar lavage (lung rinse). These are usually multiple and bilateral, but range in size, shape and distribution. CT scan may show pulmonary cysts (not to be confused with the cyst-forms of the pathogen). Chest X-ray typically shows widespread pulmonary infiltrates. They are abnormal in about 90% of cases and are often positive before the chest X-ray becomes abnormal. Gallium 67 scans are also useful in the diagnosis. The diagnosis can be confirmed by the characteristic appearance of the chest X-ray and an arterial oxygen level (PaO 2) that is strikingly lower than would be expected from symptoms. Oxygen is less able to diffuse into the blood, leading to hypoxia, which along with high arterial carbon dioxide ( COĢ) levels, stimulates hyperventilatory effort, thereby causing dyspnea (breathlessness). In this situation, lactate dehydrogenase levels increase and gas exchange is compromised. The disease attacks the interstitial, fibrous tissue of the lungs, with marked thickening of the alveolar septa and alveoli, leading to significant hypoxia, which can be fatal if not treated aggressively. In these immunosuppressed individuals, the manifestations of the infection are highly variable. The risk of PCP increases when CD4-positive T-cell levels are less than 400 cells/μL. Also, a condition similar to acute respiratory distress syndrome (ARDS) may occur in patients with severe Pneumocystis pneumonia, and such individuals may require intubation. Pneumothorax is a well-known complication of PCP. X-ray and CT of ground glass opacities and pneumothorax in pneumocystis pneumonia. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
